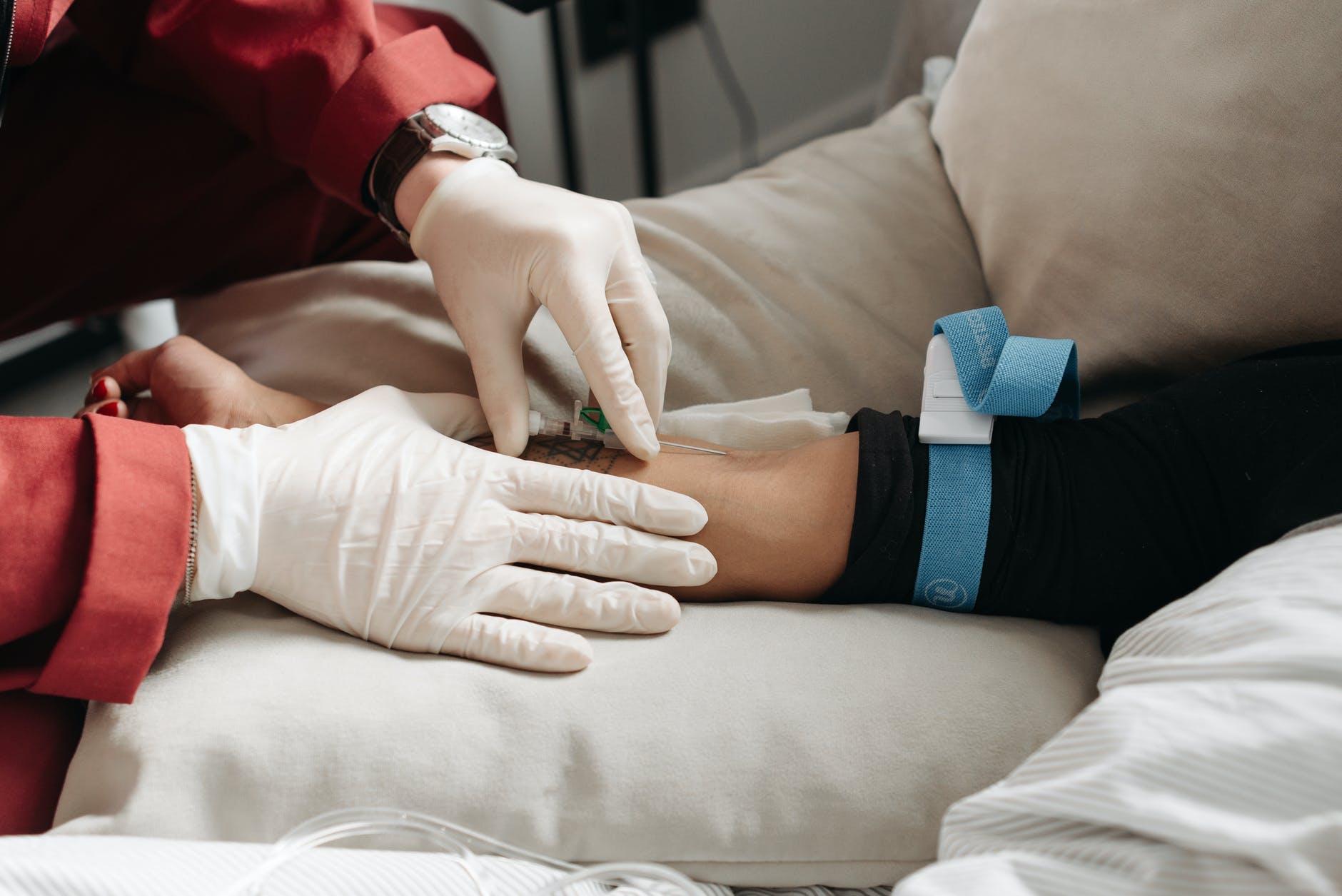
Haemostasis is the process of changing blood from a fluid to a solid-state to reduce blood loss after vessel injury.
Haemostasis also involves maintaining blood in a fluid state when there is no injury.
Haemostatic balance is maintained by regulating levels of procoagulants which promote coagulation, anticoagulants which inhibit coagulation and fibrinolysis which is the breakdown of fibrin in blood clots.
Primary haemostasis
Primary haemostasis involves the formation of the primary platelet plug which is the initial response the body has to vessel damage.
When vessels get damaged, platelets first adhere to collagen that has been exposed in the subendothelial matrix.
This binding can be done directly via glycoprotein receptors but also indirectly via Von-Willebrand factor, which is a coagulation factor that binds to the subendothelial collagen and then to receptors on the platelets.
After adhesion, platelets become activated which allows them to recruit and activate other platelets by releasing adenosine bisphosphate.
The platelets also release serotonin and thromboxane A2 which increase vasoconstriction and causes more platelets to come to the site.
The final stage of the platelet plug formation is aggregation. Aggregation refers to clumping of platelets to stop bleeding.
Fibrinogen forms bridges between activated platelets which allows them to clump together over the injured portion of the vessel.
Platelets don’t form clumps over healthy cells because the endothelial cells secrete chemicals such as nitrous oxides and other prostacyclin’s that inhibit the aggregation of platelets.
Secondary haemostasis
Secondary haemostasis involves the formation of the fibrin mesh as the platelet plug on its own is (usually) insufficient in preventing blood loss from vessel.
Formation of blood clot occurs through coagulation where blood is turned from liquid into a gel. Coagulation can be explained through the coagulation cascade.
The coagulation cascade is made of two pathways that both lead to the formation of fibrin from fibrinogen.
These two pathways are the intrinsic and the extrinsic pathways. the coagulation cascade involves several proteins known as coagulation factors that activate each other to ultimately create fibrin for the fibrin mesh.
The intrinsic pathway begins with factor 12 which gets converted into its active form (factor 12a written as XIIa) when it encounters a negatively charged surface such as the surface of an activated platelet.
A series of reactions then occur where coagulation factors are activated by other coagulation factors to ultimately convert prothrombin to thrombin.
thrombin then converts fibrinogen to fibrin which is used in the formation of blood clots.
The extrinsic pathway on the other hand begins with the release of tissue factor from damaged tissue.
Factor 7 is converted to 7a. the activated factor 7 then reacts with tissue factor to convert factor 10 to 10a.
The pathway then proceeds like the intrinsic pathway to eventually create fibrin. Thrombin has a positive feedback effect on the cascade.
It accelerates productions of factors 11a, 8a and 5a which amplifies the cascade to produce enough fibrin.
note: coagulation factors are usually written in roman numerals. I have represented them in numbers for simplicity sake
![[MacOS Error] – Compressor does not support running in a macos virtual machine](https://cdn-0.ghoopi.com/wp-content/uploads/2023/09/img_6688-150x150.jpg)