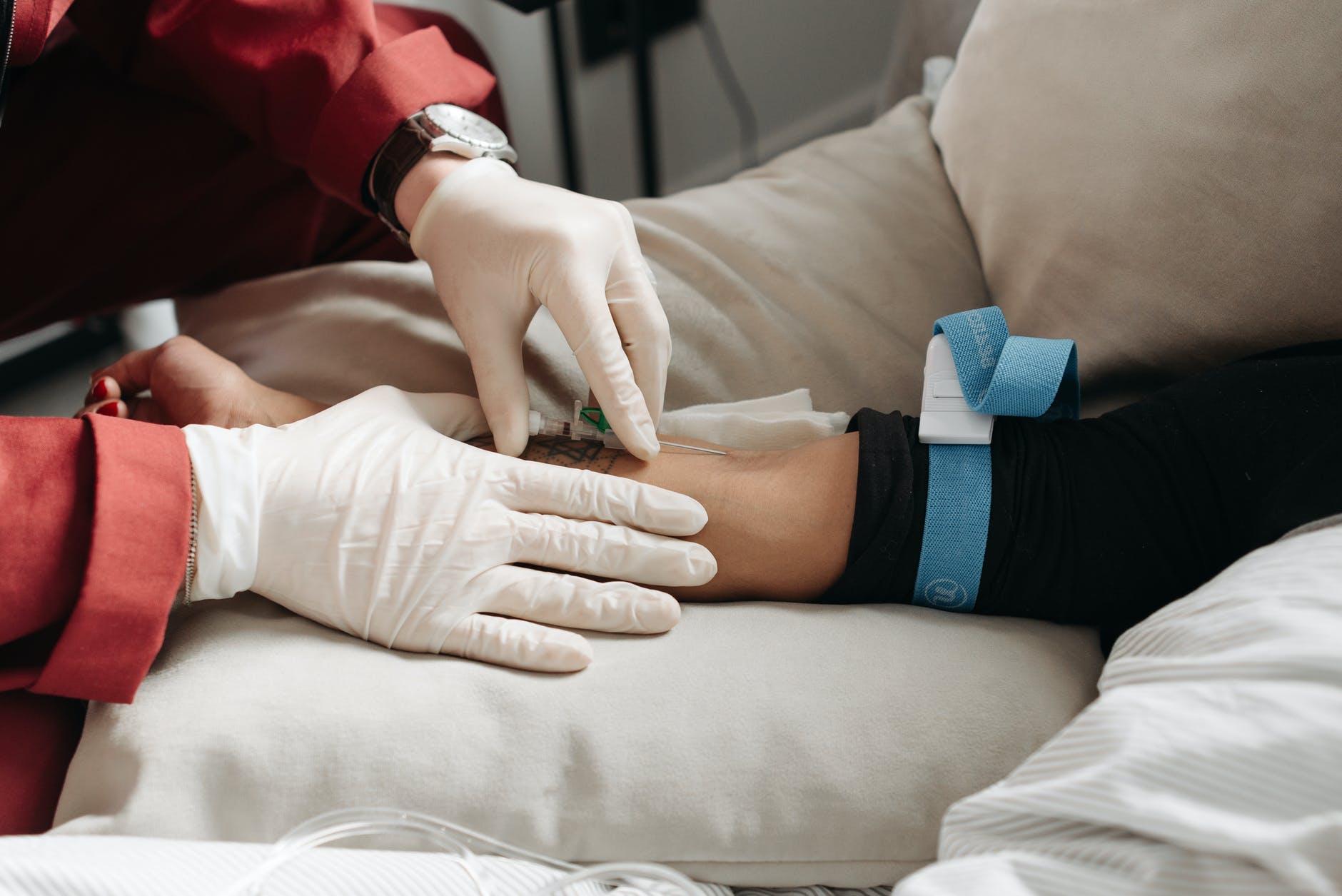
Xigris also known as Drotrecogin alfa (Activated) was a drug marketed by Eli Lilly (a drug company) and was used for the treatment of severe sepsis.
Activated protein C and sepsis were reported to go hand in hand (cure and disease respectively) however through other scientists trying to replicate the original study, they found out that the results were not very reproducible at all making the eli lilly report seem very questionable indeed.
Sepsis occurs when the body’s response to infection causes injury to its own tissue and organs.
Sepsis that includes dysfunction in one or more organs is classed as severe sepsis.
sustained inflammation seen during sepsis drives the body towards a prothrombotic (forms blood clots easier) and antifibrinolytic state (breaks down blood clots slower) which leads to blood clots forming in and blocking microvasculature which are the smaller blood vessels.
This can manifest as MODS (multiple organ dysfunction syndrome) and DIC (disseminated intravascular coagulation) and ultimately death.
Xigris is a recombinant form of activated protein C. “Recombinant” refers to the fact that the protein is artificially made from the genetic recombination of DNA.
“Activated” refers to the fact that protein C is normally inactive during circulation (zymogen) and must be activated to work.
Protein C is activated when thrombin (which converts fibrinogen into fibrin to form blood clot) binds to thrombomodulin.
When thrombin binds to thrombomodulin, thrombin loses the ability to convert fibrinogen to fibrin.
In sepsis, thrombomodulin is strongly downregulated, therefore there is less protein C being activated, and higher levels of coagulant activity due to greater thrombin activity.
APC aims to treat severe sepsis by decreasing coagulation activity, decreasing inflammation which is caused as a result of infection, and increasing fibrinolysis which is the breakdown of blood clots.
Decreasing coagulation
APC decreases coagulation by inactivating factors Va and VIIIa. These coagulation factors are required for the activation of factor X and the subsequent generation of thrombin from prothrombin.
Thrombin is a serine protease responsible for cleaving fibrinogen (soluble) into fibrin, the insoluble fibrous mesh that platelets are embedded in to form blood clots.
Decreasing inflammation
During infection and in tissue damage, an acute inflammatory response occurs.
This is due to leucocytes such as neutrophils secreting cytokines and chemokines that increase vascular permeability, promoting formation of a leucocyte rich exudate.
Protein C decreases inflammation by inhibiting cytokine production, neutrophil activation and endothelial damage.
Increasing fibrinolysis
APC promotes fibrinolysis through the inactivation of plasminogen activator inhibitor-1.
Plasminogen is the inactive precursor to plasmin, the enzyme responsible for the degradation of fibrin in blood clots.
APC also inhibits the activation of thrombin-activatable fibrinolysis inhibitor (also known as carboxypeptidase B2).
This protein usually reduces fibrinolysis by cleaving certain fibrin residues (fibrin C-terminal residues) that are important in the binding and activation of plasminogen.
Effectiveness of Xigris
Several clinical trials have been carried out into the effectiveness of Xigris in the treatment of severe sepsis and septic shock.
This includes the original PROWESS study that cited a 6% reduction (P=0.005) in the absolute risk of death in patients treated with recombinant APC (rAPC/Xigris) vs patients on placebo.
This (statistically) significant reduction in mortality suggested Xigris had an unequivocally beneficial effect on patients suffering from severe sepsis.
Subsequent trials performing the same experiments however failed to replicate the results obtained from the original PROWESS trial, raising concerns about the reliability of the study.
ADRESS was a study published in 2005 focusing on Xigris efficacy in treating adults with severe sepsis and a low risk of death.
The results surprisingly showed a greater death rate in patients treated with Xigris (18.5%) as opposed to placebo (17.5).
this however was not statistically significant with a P value of 0.34 that indicated a high degree of chance could be at play.
Shortly after, a study known as RESOLVE investigated the benefits of DAA in the treatment of children with severe sepsis).
These results were also in disagreement with the original PROWESS study as it showed very little difference in the mortality rates between the two groups (placebo = 17.5% | Xigris = 17.2%).
Treatment was administered in the same way as the PROWESS trials, however the results from this study showed no increased benefit of Xigris treatment in severe sepsis.
Amidst the controversy, the original conductors of the PROWESS study group, funded by Eli Lilly, decided to run another trial in an attempt to resolve conflicting reports.
The PROWESS-SHOCK study looked into Xigris’ efficacy against patients with septic shock.
The results showed a 2.2% absolute increase in risk of death when using Xigris as opposed to a placebo. This wasn’t statistically significant, but it was still wildly different from the claims of a 6% drop in risk of death.
The results of the PROWESS SHOCK study confirmed that Xigris had no beneficial effect in treatment of severe sepsis and septic shock.
The original PROWESS study was the only major study that showed a statistically significant decrease in mortality rate upon treatment with Xigris.
ADRESS, RESOLVE, AND PROWESS-SHOCK all showed no significant difference in mortality rates.
The differences in results from different trials may well have been down to clinical heterogeneity (differences in the trial setup) but the lack of reproducible results showing Xigris’ efficacy led to the withdrawal of Xigris in the treatment of severe sepsis.
![[MacOS Error] – Compressor does not support running in a macos virtual machine](https://cdn-0.ghoopi.com/wp-content/uploads/2023/09/img_6688-150x150.jpg)